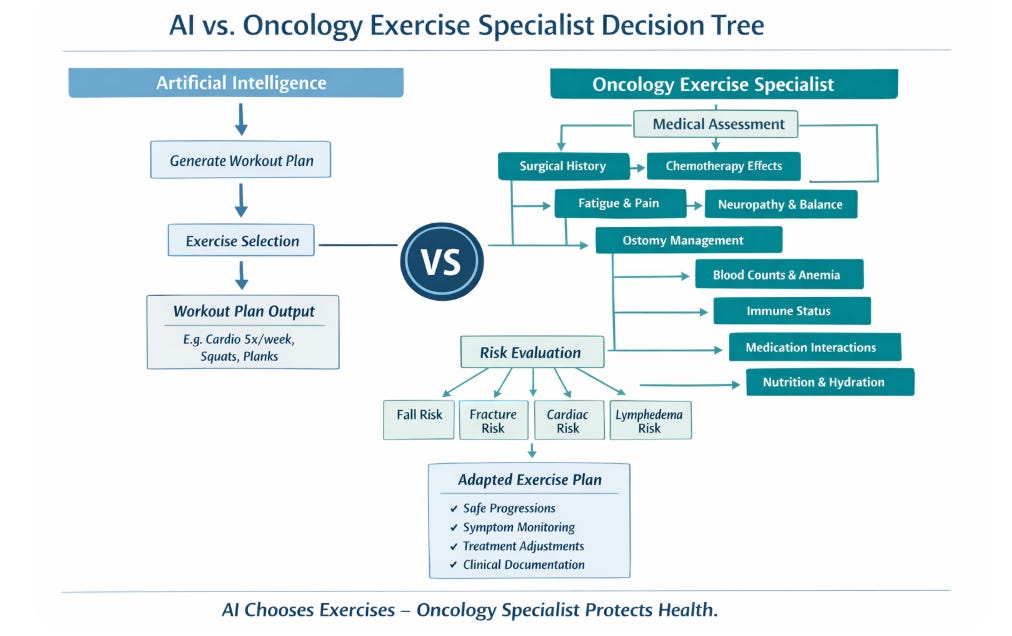
Artificial Intelligence, Professional Responsibility, and the Standard of Care in Oncology Exercise Programming
The rapid emergence of artificial intelligence (AI) tools has transformed many industries, including health, fitness, and wellness. Within seconds, AI systems can generate exercise programs, training templates, and periodized workout plans based on simple user prompts. While these tools may provide general fitness ideas, their increasing use in clinical and medically complex populations raises serious professional, ethical, and legal concerns.
One population for which exercise programming requires exceptional clinical awareness is individuals undergoing or recovering from cancer treatment. Cancer patients frequently experience profound physiological, neurological, and musculoskeletal changes related to surgery, chemotherapy, radiation therapy, immunotherapy, and hormone treatments. These changes require careful screening, specialized programming strategies, and continuous monitoring.
Artificial intelligence systems, regardless of their sophistication, are not capable of independently assessing patient-specific medical risk, treatment toxicity, or surgical complications. As a result, reliance on AI-generated exercise prescriptions without appropriate professional education may expose both the patient and the fitness professional to unnecessary risk.
Cancer Exercise Programming Is Fundamentally Different From General Fitness
Cancer exercise programming differs substantially from traditional fitness programming because cancer treatments can significantly alter physiology and physical capacity. Medical treatments used to treat cancer may impact cardiovascular function, immune status, bone density, neurological function, and tissue integrity.
Chemotherapy can result in cardiotoxicity, peripheral neuropathy, and profound fatigue. Radiation therapy can lead to fibrosis, reduced tissue elasticity, and long-term vascular changes. Surgical procedures frequently alter lymphatic drainage pathways, increase the risk of lymphedema, and permanently change biomechanical function.
Because of these treatment-related changes, exercise professionals must understand when exercise is appropriate, when it must be modified, and when it should be temporarily avoided. Improper programming may contribute to complications such as lymphedema exacerbation, fractures in individuals with compromised bone density, wound complications following surgery, severe fatigue episodes, or cardiovascular stress beyond safe limits.
For these reasons, oncology exercise is recognized as a specialized clinical discipline that requires targeted education and training.
Limitations of Artificial Intelligence in Oncology Exercise Programming
Artificial intelligence tools are typically trained on large generalized datasets rather than medically curated oncology-specific clinical information. As a result, AI systems cannot evaluate many of the critical factors that determine whether exercise programming is safe for a cancer patient.
These factors may include the presence of bone metastases, tumor location, recent surgical procedures, chemotherapy-related cardiotoxicity, immunosuppression, radiation-related tissue damage, and neurological complications. While AI-generated exercise routines may appear reasonable in a general fitness context, they cannot replace the professional judgment required to safely work with medically complex individuals.
Equally important, artificial intelligence systems do not assume responsibility for the outcomes associated with their recommendations. Responsibility ultimately rests with the professional implementing the program.
Legal and Professional Liability Considerations
From a legal standpoint, reliance on AI-generated exercise programs does not replace the requirement that professionals meet the accepted standard of care for the population they serve.
In the event that a cancer patient experiences injury or adverse outcomes during an exercise program, courts typically evaluate whether the professional possessed appropriate education, credentials, and competency related to the medical population they were serving.
Courts generally examine whether the professional demonstrated reasonable clinical judgment and whether they had received appropriate training related to the condition of the client. Stating that an exercise program was generated using artificial intelligence is unlikely to provide legal protection or reduce liability. The responsibility for program design and implementation remains with the professional.
The Role of Specialized Oncology Exercise Education
The Cancer Exercise Training Institute (CETI) developed the OncoVie® Cancer Exercise Specialist Program to address the critical gap between medical cancer treatment and safe physical recovery.
Since its introduction in 2004, the program has educated health and fitness professionals worldwide on evidence-based methods for safely and effectively working with individuals during and after cancer treatment.
The curriculum provides comprehensive instruction on cancer biology, treatment side effects, exercise contraindications, screening procedures, and condition-specific programming modifications. Professionals are also trained to recognize clinical warning signs, collaborate appropriately with healthcare providers, and implement exercise interventions that prioritize patient safety while supporting recovery, functional capacity, and quality of life.
Release of the 15th Edition of the OncoVie® Cancer Exercise Specialist Handbook
As cancer treatment continues to evolve, oncology exercise education must remain aligned with the most current scientific and clinical evidence.
In response to rapidly advancing medical treatments and survivorship research, CETI is releasing the 15th Edition of the OncoVie® Cancer Exercise Specialist Handbook, which incorporates extensive updates reflecting developments in 2025 and 2026 across multiple areas of cancer care.
This updated edition includes expanded coverage of current research in exercise oncology, modern surgical procedures and post-operative considerations, advances in chemotherapy, immunotherapy, and targeted therapies, and the long-term physiological implications of these treatments.
In addition, the handbook includes updated information on nutritional strategies that support recovery and inflammation management, emerging integrative and complementary medical approaches used in oncology care, and updated screening and risk-management protocols for fitness professionals working with cancer populations.
These updates ensure that professionals completing the program are equipped with the most current scientific, medical, and practical knowledge available for safely guiding cancer patients through exercise participation.
Artificial Intelligence as a Supplementary Tool
Artificial intelligence technologies may serve as useful supplementary tools for brainstorming exercise programming ideas or organizing training concepts. However, these tools should not replace professional education, clinical awareness, or responsible decision-making when working with medically vulnerable populations.
In oncology exercise, the expertise of the trained professional remains the primary safeguard for patient safety. Technology may assist the professional, but it cannot substitute for the specialized education required to interpret complex medical conditions and treatment histories.
The Growing Need for Oncology Exercise Professionals
The global population of cancer survivors continues to grow as medical treatments improve and survival rates increase. Exercise is now widely recognized as a critical component of supportive cancer care, contributing to improvements in functional capacity, fatigue management, treatment tolerance, and quality of life.
Hospitals, rehabilitation centers, and fitness facilities increasingly require professionals who possess appropriate education in oncology exercise programming. Professionals who pursue specialized training not only enhance patient safety but also position themselves as leaders in an expanding area of healthcare-integrated fitness services.
Professional Responsibility and the Future of Oncology Exercise
Health and fitness professionals who wish to work responsibly with individuals affected by cancer are strongly encouraged to pursue formal oncology exercise education.
The CETI OncoVie® Cancer Exercise Specialist Program provides the clinical framework, evidence-based methodology, and practical tools required to safely support patients during and after cancer treatment.
With the release of the 15th Edition of the OncoVie® Cancer Exercise Specialist Handbook, professionals now have access to the most current research, clinical insights, and applied exercise strategies available in the field of oncology exercise.
Through appropriate education, careful clinical judgment, and adherence to evidence-based practice, fitness professionals can play an important role in improving recovery, functional capacity, and quality of life for individuals living with and beyond cancer.
Premium Subscriber Bonus
AI vs Clinical Judgment in Oncology Exercise
Detailed Case Application Template: Colon Cancer, Standard Treatment, Ileostomy, and Exercise Decision-Making
This premium resource is designed to show, in practical terms, where artificial intelligence may be useful as a secondary support tool and where it is clearly inadequate without formal oncology exercise education. Cancer exercise prescription requires interpretation of diagnosis, surgery, treatment toxicities, functional limitations, nutrition-related complications, and symptom variability. Current guidance supports exercise during and after cancer treatment, but it also emphasizes individualized clinical judgment, screening, and modification rather than generic programming.
In colorectal cancer, that need for judgment becomes even more important when the client has undergone bowel surgery, is receiving oxaliplatin-based chemotherapy, and is living with an ileostomy. Ileostomy formation is associated with dehydration and electrolyte disturbance risk, and chemotherapy-induced peripheral neuropathy can affect gait, balance, and exercise safety. Exercise is beneficial, but the professional must determine not only what the client can do, but what they should avoid, what needs modification, and what requires medical follow-up.